This article contains affiliate links. We may earn a small commission at no extra cost to you.
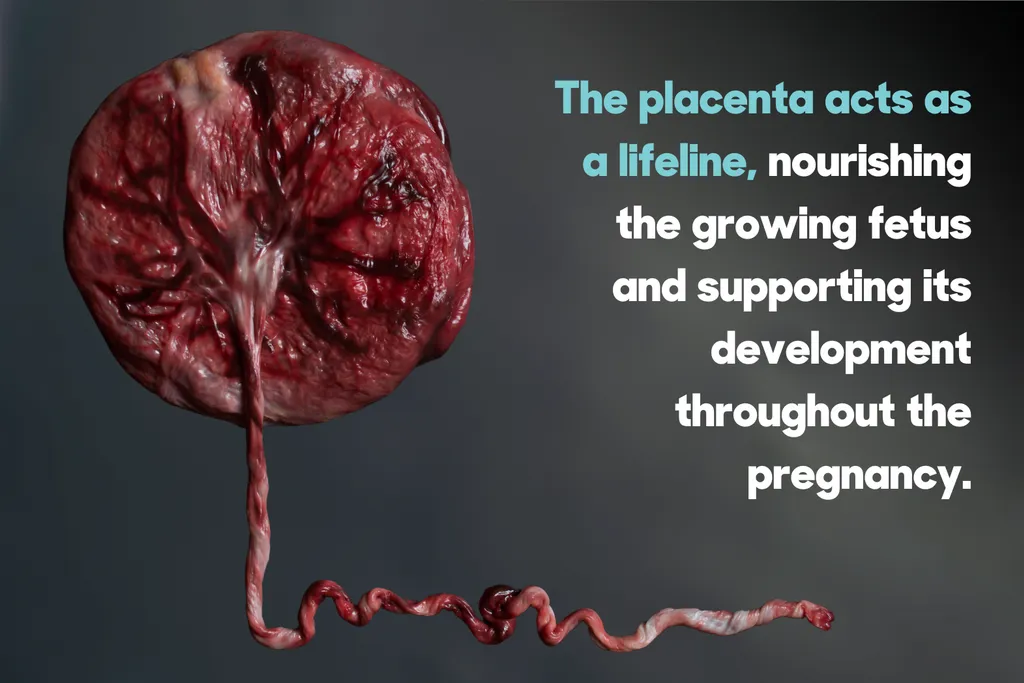
The moment a woman delivers her baby, something else leaves her body.
It gets quietly removed. Placed in a biohazard bag. Labeled medical waste. She is not asked what she wants done with it. She is rarely told what will happen next.
What happens next, in many hospitals, is that it gets sold.
Not by her. She cannot sell it — that is illegal. But the hospital can. The procurement company can. The biotech firm that processes it into stem cell therapies, wound-healing grafts, anti-aging serums, and cancer treatments can. The pharmaceutical industry building a billion-dollar market on the back of it can.
She just can't.
The Market She Doesn't Know She's In
The global placenta market was valued at approximately $652 million to over $1.3 billion in 2025, depending on which segment you measure — and it is projected to more than double by 2032 across most estimates.
That is the conservative figure. Some analysts tracking the broader placental bioeconomy — including pharmaceutical applications, regenerative medicine, cosmetics, and nutraceuticals — put the combined value of placenta-derived products significantly higher. The market is growing at close to 9% annually. Investors are flooding in.
Placental tissues are becoming of great interest to pharmaceutical and biotechnology companies that are willing to use them to develop drugs and use them as therapeutic agents. Companies like Celularity — which raised $250 million and listed on Nasdaq — are building entire business models around placenta-derived cell therapies targeting cancer, Parkinson's disease, Crohn's disease, and multiple myeloma.
The woman who produced the raw material is not a shareholder. She is not a supplier. She is not a partner in any legal sense.
She is the source. That is all.
Women whose placentas are used by companies do not receive compensation or recognition — and in most instances won't be able to afford the cures or treatments developed from their own bodies.
— HuffPost UK, on the placenta bioeconomy
Why You Can't Sell Your Own
The legal landscape is deliberately confusing — and that confusion benefits the people profiting from it.
In the United States, the National Organ Transplant Act (NOTA) prohibits the sale of human organs. The question of whether the placenta is legally an organ has never been adjudicated in court. The common law tradition at hospitals is to treat the placenta like other tissues produced as a byproduct of surgery — as human pathological waste.
And this classification is extraordinarily convenient for the hospitals.
The current system where hospitals categorize the placenta as waste is convenient for them, because it allows hospitals to give or sell this "waste" to procurement organizations and medical product companies.
In other words: it is waste when you want it. It is a commercial product when someone else does.
Some hospitals have come under fire when it was revealed that they were selling discarded placentas to biomedical companies. One researcher pointed out, with slight hesitancy, that research hospitals could have a financial motive to keeping women's placentas given that "a lot of bigger hospitals have — or, at least, had — contracts with pharmaceutical and cosmetic houses to sell the placentas."
The hospitals denied it. The biotech companies said nothing. The women were never asked.
The C-Section Question Nobody Wants to Answer
Here is where the story gets more uncomfortable.
The global C-section rate has roughly doubled since 2000. The prevalence of cesarean section worldwide increased from about 16 million in 2000 to 29.7 million in 2020. The WHO recommends a rate of 10–15%. Most developed nations are significantly above it. The U.S. sits at around 32%. Brazil's private hospitals exceed 80% in some regions. India's private facilities now perform C-sections in more than half of all deliveries.
Everyone agrees this is a problem. The explanations offered are familiar: physician convenience, fear of litigation, scheduling preferences, maternal anxiety.
What is discussed far less often is that C-section placentas are, for certain biotech applications, preferable.
Placental tissues collected under controlled surgical conditions — as in elective C-sections — allow for a complete and sterile chain of custody from collection in a controlled medical environment to processing in a licensed lab. A planned, scheduled surgery produces a cleaner, more intact specimen than an emergency procedure or a prolonged vaginal labor. The tissue quality matters. The cell yield matters. The sterility matters.
And research confirms that financial incentives are already driving unnecessary C-section rates globally.
Doctors who perform C-sections, a surgery that takes about 45 minutes, usually get paid more than those who patiently await vaginal birth, a process that can take hours or days. Hospitals, which also bill more for the surgeries, lack motivation to demand accountability from doctors on staff, which likely incentivizes the procedure.
More money for the surgery. Better tissue for the biotech pipeline. Rising C-section rates globally.
No one is drawing this line directly. But the line is there.
High cesarean rates are frequently driven by non-medical factors such as maternal requests, convenience, financial incentives, medico-legal concerns, and physician preferences rather than medical necessity. The question of whether placenta value is one of those financial incentives has not been studied. That absence of study is itself worth noting.
What Most People Don't Know About This
Most women who give birth in hospitals have never been told any of this.
They sign consent forms at the point of admission that bundle tissue disposal into general medical consent. They are not shown a separate document explaining that their placental tissue may be transferred to a procurement organization. They are not informed that tissue from that organization may end up in a pharmaceutical product or a clinical trial. They are not told what their tissue is worth commercially.
Most women sign generic consent forms that mention "tissue disposal," but rarely spell out potential commercial use. Hospitals often bundle tissue consent with general medical consent, making it easy to miss. Mothers almost never receive compensation or even acknowledgment for their donation.
There is a direct legal parallel here that nobody in the mainstream conversation mentions: Henrietta Lacks.
In 1951, cells were taken from Henrietta Lacks during a medical procedure without her knowledge or consent. Those HeLa cells became the most widely used human cell line in medical history — generating billions of dollars in commercial value across decades of research. Her family received nothing. She was never asked.
The placenta system is the same structure, running quietly, at every maternity ward in the country, every single day.
What most people also don't know: in many states, you cannot even take your own placenta home without navigating a complex, hospital-specific bureaucracy.
Across the United States, there is a patchwork of policies at different levels, down to individual hospitals and medical practices, which effectively constitute a "hidden form of placenta law." At the time your baby is delivered, whether or not you can repossess the placenta may come down to where you delivered the baby and who is the staff on duty that day.
You produced it. They decide what happens to it.
Recommended Reading
The Immortal Life of Henrietta Lacks by Rebecca Skloot
The definitive account of what happens when the medical system takes tissue from a woman's body without her knowledge and builds a billion-dollar industry on it. If the placenta story made you uneasy, this book will show you how deep the pattern goes.
Check price on AmazonWhy This Still Matters Today
The placenta market is not a niche concern. It is a $1.3 billion industry growing at nearly 10% per year, built almost entirely on tissue collected from women who are not compensated, not fully informed, and — in the United States at least — not legally permitted to participate in the commercial upside they generate.
The companies benefiting from this are publicly listed. Their executives are household names in biotech. Their investors include Silicon Valley's most prominent venture funds. And the women supplying the raw material are handing a bill for giving birth.
This matters because the placenta is not uniquely valuable as a curiosity. It is a primary source of mesenchymal stem cells — cells with the ability to differentiate into bone, cartilage, fat, and muscle tissue — that researchers believe could eventually treat Parkinson's disease, spinal cord injuries, diabetes, multiple sclerosis, and a growing list of conditions currently without effective cures. The commercial pipeline being built on these cells will generate tens of billions in value over the coming decades.
And none of that pipeline acknowledges the women at its origin.
The C-section question matters for the same reason. The financial incentives driving unnecessary surgical deliveries are already documented and well-studied. The additional financial incentive of producing higher-quality placental tissue in a scheduled surgical environment has not been studied. It should be. A system that already overpays for surgeries that also happen to produce more commercially valuable tissue is a system with a conflict of interest that nobody is naming out loud.
Unnecessary C-sections result in elevated rates of maternal and infant morbidity and mortality and have high financial costs. They also — incidentally, or perhaps not so incidentally — produce placentas in the precise condition that biotech procurement organizations prefer.
The questions worth asking are not complicated.
Does your hospital have a contract with a tissue procurement organization? What consent do you actually sign regarding your placental tissue? Who profits from it? Can you opt out?
Most women never think to ask. Most hospitals are not volunteering the answers.
That asymmetry of information — where the institution knows what your tissue is worth and you do not — is not an accident. It is the architecture of the system.
The Point
A billion-dollar industry is built on tissue taken from women who are told it is waste. The women cannot sell it. The hospital can. The biotech company can. The pharmaceutical firm turning it into cancer treatments can. And C-sections — which produce cleaner, more commercially valuable tissue — are rising globally, driven partly by the same financial incentives that have always shaped how women's bodies are treated in medicine. None of this is a conspiracy. All of it is a system. And the first step to changing a system is knowing it exists.
Sources
- 360iResearch — Placenta Market Size & Share 2025–2030 — 360iresearch.com
- Parents Guide to Cord Blood — Can You Sell Your Baby's Placenta? — parentsguidecordblood.org
- Vice — Hospital Regulations Are Forcing Women to Steal Their Own Placentas — vice.com
- HuffPost UK — BioTech: Profiting From Women's Bodies Without Their Consent — huffingtonpost.co.uk
- Scientific American — C-Section Rates Are Way Too High. We Need to Hold Doctors and Hospitals Accountable — scientificamerican.com (Feb 2025)
- PMC / Frontiers in Global Women's Health — Global increased cesarean section rates and public health implications — pmc.ncbi.nlm.nih.gov
- Leapfrog Group — C-Section Awareness Month 2025 Maternity Care Report — leapfroggroup.org
- Berry Good Life — The Placenta Pipeline: How Women's Birth Tissues Became Big Business — berrygoodlife.us